In this week's edition
- ✍️ Letter from P'Fella
A monthly deep dive: Building a focused plastics journal - 🖼️ Image of the Week
Supermicrosurgical exposure in lymphaticovenular anastomosis - 🚑 Technique Tip
Supermicrosurgical lymphovenous anastomosis (LVA) - 📖 What Does the Evidence Say?
Supermicrosurgery for lymphedema: When is LVA enough? - 🔥 Articles of the Week
LVA for lymphedema, SEATTLE technique, & supermicrosurgery in lower limb recon: 3 articles with 1-sentence summaries. - 💕 Feedback
Suggest ideas & give feedback!
A Letter from P'Fella
A Monthly Deep Dive: Building a Focused Plastics Journal
A while ago, we spoke about building a monthly newsletter. Similar to this Plastics Paper that comes to your inbox, but more in-depth, more structured, and more like a journal than a newsletter.
While the idea has always been exciting, we didn't want it becoming more content rather than better learning.
And because we've been speaking to a few of you over the past couple of weeks, we are getting more face-to-face insights on how people actually learn plastic surgery. The problem isn’t a lack of information. It’s that most of it doesn’t go far enough.
You read something, you recognise it, you move on, but you don’t always get to the point where you can actually use it. And that gap only really shows itself when you’re in theatre, or on call, or trying to make a decision under pressure. That’s the gap we’re trying to solve.
So instead of building a “monthly newsletter” in the traditional sense, we’re thinking about a better way for you to absorb what you learn here.
What if we created a monthly, specialised edition of a journal? One that focuses on a single area, and goes properly deep on it. The goal isn't to make it busier, rather more deliberate.
Something that takes a topic and breaks it down in a way that actually gets you thinking:
- How to approach it
- How decisions are made
- Where things may go wrong
- What people don’t usually explain, but expect you to know
The kind of journal paper you could read once, and then come back to before a case or a teaching session.
We’ve been brainstorming where to start, and one area that kept coming up is hand surgery. It’s one of those cases where having a clear mental model makes a huge difference to how confident you feel approaching it.
As always, we wanted to come to you before we go ahead and build this. Because our goal is to create something you’d actually read and come back to 👉
With love,
P’Fella ❤️
Image of the Week
Supermicrosurgical Exposure in Lymphaticovenular Anastomosis
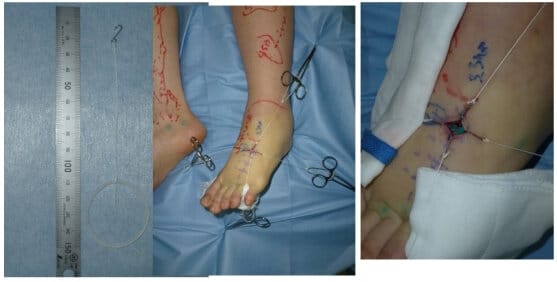
This week's image demonstrates lymphaticovenular anastomosis (LVA) using hook-type retractors to stabilise a small operative field. In supermicrosurgery, vessels are often <0.8 mm, and even minimal movement can compromise precise suturing.
The incision is typically just 1-2.5 cm, requiring fine retraction to maintain exposure without obstructing the field. Here, multiple micro-hooks create a stable, tension-free window, allowing accurate dissection and intima-to-intima anastomosis under the microscope.
This image highlights a key principle: control of the operative field is critical when working at the limits of vascular repair.
Technique Tip
Supermicrosurgical Lymphovenous Anastomosis (LVA)
This video demonstrates lymphovenous anastomosis (LVA) performed at the supermicrosurgical level, connecting submillimetre lymphatic channels to venules to bypass lymphatic obstruction. The key challenge is the fragility and collapse-prone nature of lymphatics, requiring meticulous handling and precise lumen identification under high magnification.
The core technical principle is atraumatic manipulation and exact intima-to-intima alignment. Gentle dilation of the lymphatic, minimal handling, and precise suture placement are essential to avoid tearing or thrombosis. Successful anastomosis is confirmed intraoperatively by visualisation of flow across the junction, often seen as movement at the lymph-blood interface, a critical indicator of patency in supermicrosurgery.
What Does the Evidence Say?
Supermicrosurgery for Lymphedema: When Is LVA Enough?
That pattern is reflected in clinical outcomes. In prospective breast cancer-related lymphedema series, supermicrosurgical LVA reduced limb-volume difference and improved quality of life at 6-12 months, with over half of patients in one study able to stop compression garments. Comparative cohort data also suggest that microsurgical treatment outperforms decongestive therapy, but that vascularized lymph node transfer (VLNT) may produce greater improvement in circumference, reduction rate, and cellulitis burden than LVA alone; adding microvascular breast reconstruction did not further improve lymphedema outcomes.
Practical Takeaway: LVA is most convincing in early disease with functional lymphatics, while VLNT becomes more attractive when disease is more advanced or bypass alone is unlikely to be enough.
Sources: (Koshima, 2013); (Hong, 2018); (Badash, 2018); (Winters, 2017); (Engel, 2017)
Articles of the Week
3 Interesting Articles with One-Sentence Summaries
Supermicrosurgical lymphaticovenular anastomosis produced far greater limb reduction than bandaging alone, establishing the key principle that lymphedema can be treated by restoring lymphatic outflow rather than relying on compression alone.
Temporary lymphatic expansion increases vessel diameter and significantly improves success rates of side-to-end lymphaticovenular anastomosis, reinforcing that in supermicrosurgery, small technical modifications can determine whether submillimetre anastomoses succeed or fail.
Perforator-to-perforator anastomosis expands recipient vessel options while reducing dissection and major vessel sacrifice, demonstrating that supermicrosurgery shifts reconstruction toward smaller vessels with equivalent reliability and less morbidity.


