In this week's edition
- ✍️ Letter from P'Fella
Why burns education matters more than it gets credit for - 🤓 The Sunday Quiz
Still renovating! - 🖼️ Image of the Week
Hand escharotomy: Restoring perfusion - 🚑 Technique Tip
Split-thickness skin grafting for burn coverage - 📖 What Does the Evidence Say?
Can we reduce “procedural burden” without compromising care? - 🔥 Articles of the Week
Dermal substitution in burn management: 3 articles with 1-sentence summaries. - 💕 Feedback
Suggest ideas & give feedback!
A Letter from P'Fella
Why Burns Education Matters More Than It Gets Credit For
Because the moments that matter are high-stakes, and the exposure is patchy. You can do months of training without seeing the right case at the right time, with someone who explains why they’re doing what they’re doing.
So you end up with a weird gap in surgical education: We all agree burns are important ... but many surgeons feel under-trained in them.
The Part of Burns People Underestimate
Most people think “burns education” is about the acute phase: TBSA, fluids, escharotomy, dressings, infection, and when to transfer.
That stuff is important. But it’s not the bit that quietly causes the most long-term harm. The harder part is what comes after. Late reconstruction. Contractures. Scar patterns that tighten over months. Hands that lose web spaces. Necks that won’t extend. Eyelids that drift. Joints that stiffen. Kids who grow into their scars.
What Good Burns Education Should Look Like
Burns education needs a different rhythm compared with higher-volume conditions.
It has to be structured and revisitable, because you won’t see enough cases for repetition to do the work for you. Burns needs a system, not just content.
Why We’re Investing in This Now
This week’s issue is burns-focused for a reason.
We’re putting real energy into building burns education that’s practical, clear, and usable. Because if we can make burns feel more teachable, it raises the baseline for everyone: trainees, generalists, and specialists.
Behind the scenes, we’re building an internal Burns Department: a small team whose job is to keep this area sharp, current, and clinically honest. We’ve got expert input lined up (more on that soon), and we’re now looking for a few people with a genuine burns interest to help us pressure-test and strengthen what we build.
If burns is something you care about... whether you’re early in training or you’ve been doing this for years....applications are open to join our team!
Because good burns education shouldn’t depend on luck. It should depend on good systems.
If you haven't already, let us know you're interested below. We'll reach out soon!
With love,
P’Fella ❤️
The Sunday Quiz
Still Renovating!
Image of the Week
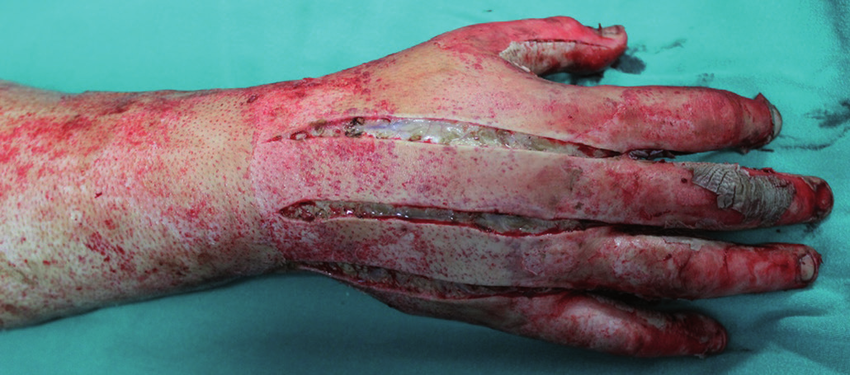
Hand Escharotomy: Restoring Perfusion
This image shows a dorsal hand escharotomy performed for a circumferential full-thickness burn. In deep burns, the rigid eschar acts as a constricting band, raising tissue pressure and compromising digital perfusion.
Incisions are taken through the eschar to the subcutaneous tissue, with extensions through the interdigital spaces to decompress the interosseous compartments and restore blood flow.
👉 Escharotomy relieves the constricting burn and restores perfusion before irreversible tissue damage occurs.
Technique Tip
Split-Thickness Skin Grafting for Burn Coverage
Deep partial- and full-thickness burns often require tangential excision followed by split-thickness skin grafting (STSG) to achieve early wound closure. In this procedure, the epidermis and a portion of the dermis are harvested from a donor site using a dermatome and transferred to the prepared wound bed, allowing coverage of large defects while the donor site re-epithelialises.
Key technical principles include preparing a well-vascularised wound bed after excision of non-viable tissue, harvesting a thin, uniform graft, and securing it carefully to avoid shearing or haematoma formation. When successful, STSG enables rapid coverage of burn wounds, reduces infection risk, and accelerates healing compared with delayed closure.
What Does the Evidence Say?
Can We Reduce “Procedural Burden” Without Compromising Care?
For the procedure itself, enzymatic debridement with bromelain-based agents (e.g., NexoBrid) has randomized trial evidence showing faster time to complete debridement and reduced need for surgical excision and grafting, while reporting similar scar quality and quality-of-life outcomes compared with standard care and similar adverse-event rates. A broader evidence-mapping review of burn debridement literature supports enzymatic debridement as one of the better-supported “newer” debridement strategies, while also highlighting that the overall field still contains major evidence gaps and heterogeneity.
Bottom line: If your goal is to make burn care more tolerable and potentially less surgically intensive, the evidence supports two complementary moves: VR as a non-pharmacologic analgesic adjunct for painful wound care, and enzymatic debridement as a selective eschar-removal strategy that can reduce operative excision/grafting in appropriate deep burns — both best used within a protocolised burn-service pathway rather than ad hoc.
Sources: (Hoffman, 2008); (Maani, 2011); (Rosenberg, 2014); (Ziegler, 2020)
Articles of the Week
3 Interesting Articles with One-Sentence Summaries
A collagen-elastin dermal substitute placed beneath a split-thickness graft preserves graft take while significantly improving long-term skin elasticity and pliability in reconstructive wounds, reinforcing the principle that dermal restoration is key to functional scar quality.
Dermal substitutes in acute burn care provide a scaffold that restores dermal architecture, improving long-term functional and cosmetic outcomes while laying the foundation for regenerative strategies such as tissue engineering and stem cell–based skin replacement.
NovoSorb BTM typically requires about 4 weeks to integrate, then supports high split-thickness graft take with improving scar quality over 12 months, reinforcing temporisation plus neodermis formation when early autografting is not possible.


