In this week's edition
- ✍️ Letter from P'Fella
Before you submit - 🖼️ Image of the Week
Facial dog bite reconstruction - 🚑 Technique Tip
Dog bite wounds: Irrigation procedure - 🎓 Building in Public
Meet the pilot On-Call Team - Aesthetics - 📖 What Does the Evidence Say?
Dog bites: Primary closure and hand antibiotics - 🔥 Articles of the Week
Bite injuries and risks of infection - 💕 Feedback
Suggest ideas & give feedback!
A Letter from P'Fella
Before You Submit
A lot of you replied to that letter, which tells me the issue landed where I thought it would. Because underneath all of that is a simpler problem: a lot of people want to do research properly, but the way in still feels hidden. You’re told to publish, told it matters, and somehow still left to figure out the basics on your own. And when something feels confusing enough, someone will always find a way to package that confusion and sell it back to you.
That got me thinking about what would actually be useful here. Not another polished course with a promise that you’ll “get published.” Just something open, practical, and properly explained. The sort of thing that helps with the real questions people get stuck on.
- How do you come up with a sensible project?
- What does good methodology actually look like?
- How do you know if a study is strong enough to submit?
- How do you choose the right journal?
- What should you check before you send it off?
- What usually goes wrong after submission, and what can you do about it?
So we want to start working on something that tackles exactly that. The working idea at the moment is Before You Submit. The aim is simple. Make research feel less opaque. Give people a clearer path into it. Research should feel like something you can learn with proper guidance, honest feedback, and a bit of structure. It shouldn’t feel like a closed world where access belongs only to the people already inside it.
So, I wanted to ask you first. If we build this, what do you actually want in it? What part of research still feels unclear? What do you wish someone had explained before your first project or your first submission? Let us know below, and we’ll use that to build it properly.
With love,
P’Fella ❤️
Image of the Week
Facial Dog Bite Reconstruction
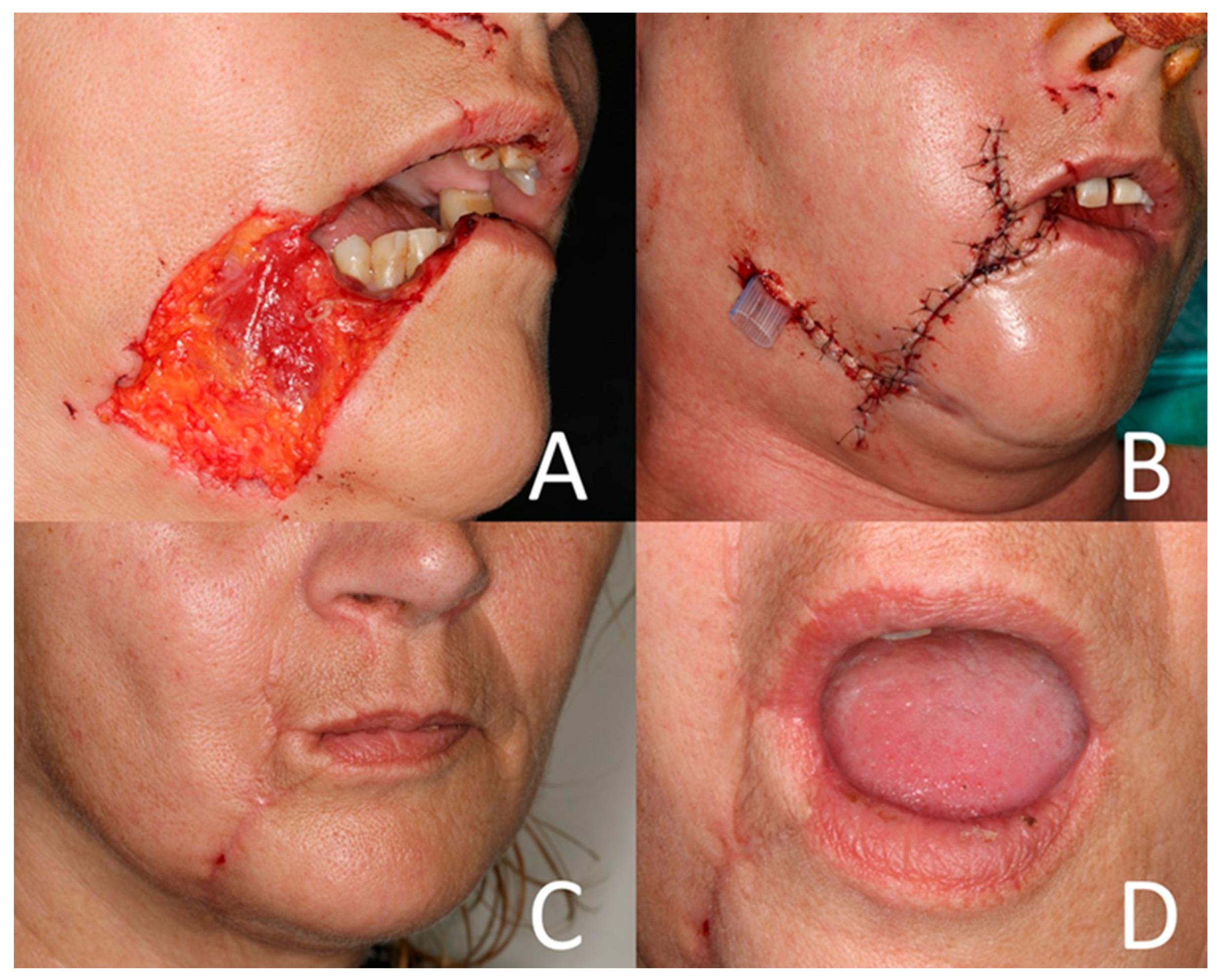
This week's image demonstrates the management of a severe perioral dog bite injury (Lackmann type III), progressing from initial soft tissue loss to reconstruction and early outcome.
The initial defect (A) shows full-thickness soft tissue loss with irregular wound edges, typical of high-energy bite injuries. Following meticulous irrigation and debridement, the wound is primarily closed with careful layered approximation and placement of a drain (B) to reduce dead space and infection risk.
At follow-up (C, D), there is good restoration of oral competence and acceptable aesthetic outcome, highlighting the capacity of facial tissues for recovery when managed early and appropriately.
Key learning points:
- Facial dog bites often involve complex, contaminated soft tissue defects
- Early thorough washout + debridement is critical
- Primary closure is frequently achievable due to robust facial vascularity
- Functional goals (oral competence) are as important as cosmesis
Technique Tip
Dog Bite Wounds: Irrigation Procedure
This video highlights one of the most important steps in dog bite management: copious irrigation. Dog bites are crush-contamination injuries with a high bacterial burden, so the priority is not immediate closure, but reducing inoculum and removing debris. High-pressure saline washout, gentle exploration, and removal of devitalised tissue are the key principles before any decision about closure is made.
Even “simple” bite wounds deserve a systematic assessment. Always examine tendon function, neurovascular status, joint involvement, and occult puncture tracts, especially in the hand. Most uncomplicated wounds can be dressed loosely and reviewed within 48 hours, while high-risk injuries (hand bites, puncture wounds, crush injury, delayed presentation, immunocompromised patients) often warrant prophylactic co-amoxiclav and closer follow-up.
Building in Public
Pilot On-Call Team - Aesthetics
This is a global group of students and junior trainees, led by Benedetta Agnelli (Clinical Lead) with expert input from Prof. Foad Nahai.
We also introduced our new backend platform, where reviewers can claim articles and provide structured feedback as part of the workflow.
This is an important step toward building a scalable and high-quality platform powered by both automation and real clinical judgement. We're super excited to see where this goes 🚀
What Does the Evidence Say?
Dog Bites: Primary Closure and Hand Antibiotics
Antibiotic prophylaxis is also better understood as selective rather than routine. Systematic-review evidence does not show a clear overall benefit for all dog bites, but it does show a meaningful reduction in infection for bites to the hand. That makes the most evidence-based approach meticulous washout, selective primary closure of appropriate wounds, and targeted antibiotics for higher-risk injuries, especially hand bites rather than blanket antibiotics for every uncomplicated dog bite.
Sources: (Maimaris, 1988); (Paschos, 2013); (Cheng, 2014); (Medeiros, 2001); (Quinn, 2010)
Articles of the Week
3 Interesting Articles with One-Sentence Summaries
Even seemingly minor human or animal bite wounds to the hand carry a high risk of polymicrobial infection due to unique anatomy and oral flora, requiring prompt irrigation, prophylactic antibiotics, and often delayed closure to prevent significant morbidity.
Seemingly trivial dog bite injuries can lead to delayed, atypical infections such as Mycobacterium kansasii tenosynovitis, requiring prolonged antimicrobial therapy and multiple surgeries for functional recovery.
Cat and dog bites introduce polymicrobial flora that can progress from local infection to severe systemic disease, including sepsis, meningitis, and endocarditis, highlighting the need for early, targeted antimicrobial management and vigilance for atypical pathogens.


